 |
 |
 |
 |
by Members of the Reforming States Group
co-published by the Reforming States Group and the Milbank Memorial Fund
May 2009
(To see a complete list of Milbank reports, click here.
To print this report, click here for the pdf version.)
Table of Contents
Access to Care
Jane Kitchel, Vice-Chair, Appropriations Committee, Vermont SenateControlling the Cost of Care
Elizabeth Roberts, Lieutenant Governor, State of Rhode IslandControlling the Cost of Care
Charles Scott, Chair, Labor, Health and Social Services Committee, Wyoming SenateQuality of Care
John Colmers, Secretary, Maryland Department of Health and Mental Hygiene, and Pam Maier, Chair, Health and Human Development Committee, Delaware House of RepresentativesStates and the Employee Retirement Income Security Act (ERISA)
S. Peter Mills, Member, Health and Human Services Committee, Maine Senate, and John Colmers, Secretary, Maryland Department of Health and Mental HygieneInsurance Market Reform
Sandy Praeger, Commissioner of Insurance for the State of Kansas, and Immediate Past President of the National Association of Insurance CommissionersLong-Term Care
John Selig, Director, Arkansas Department of Human Services, and Bruce Goldberg, Director, Oregon Department of Human ServicesMental Health and Addictive Disorders
Gene Davis, Minority Whip, Utah Senate, and Sybil Richard, Deputy Secretary, Louisiana Department of Health and HospitalsPublic Health
Richard N. Gottfried, Chair, Health Committee, New York State Assembly, and S. Peter Mills, Member, Health and Human Services Committee, Maine SenateWorkforce Development
Leticia Van de Putte, Chair, Veteran Affairs and Military Installations Committee, Texas SenateChildren’s Health and Well-Being
Kevin Concannon, Director, Iowa Department of Human ServicesHealth Disparities
Leticia Van de Putte, Chair, Veteran Affairs and Military Installations Committee, Texas Senate, and Scott Nishimoto, Vice-Chair, Health Committee, Hawaii House of RepresentativesMedical Liability Reform
Charles Scott, Chair, Labor, Health and Social Services Committee, Wyoming SenateMedical Liability Reform
Kathy Stein, Chair, Judiciary Committee, Kentucky House of RepresentativesReforming States Group (RSG) Steering Committee
Foreword
The U.S. health care system is in crisis and, in many dimensions, lags behind much of the developed world in terms of cost, quality, and access, despite spending the most for health care per capita. President Obama and the new Congress have responded to this crisis by placing health care reform high on the national priority list.
States have valuable experience and can contribute a unique perspective to the national health care reform dialogue. That’s because most have a constitutional obligation to provide for the welfare of their citizens. And each year, they raise and appropriate billions to fund a wide variety of local, state, and federal-state health care programs and regulatory activities.
With support from the Milbank Memorial Fund, the Reforming States Group (RSG) offers this report—which includes an introduction and a collection of essays written from the states’ perspective—as a guide to the new administration and Congress for health care reform. The introduction presents the RSG’s recommendations, and the essay collection provides a useful overview of a dozen key health policy topics, ranging from access to care to cost, insurance market reform to mental health, and workforce development to health disparities.
For the most part, the essays were completed before the 2009 reauthorization of the SCHIP program and prior to the passage of the American Recovery and Reinvestment Act (ARRA) earlier this year. As such, the report does not reference either bill or any corresponding federal policy changes.
Organized in 1992, the RSG is a voluntary association of leaders in health policy in the legislative and executive branches of government, from all fifty states, several Canadian provinces, Australia, and Scotland. The Milbank Memorial Fund is an endowed national foundation, established in 1905, that works with decision makers in the public and private sectors to carry out nonpartisan analysis, study, and research on significant issues in health policy.
Many individuals contributed to the preparation of this report. The members of the RSG who wrote the essays or reviewed them in draft form are listed in the acknowledgments. The following persons, who are listed in the positions they held at the time of their participation, provided advice and guidance and helped to write the introduction: John McDonough, Executive Director, Health Care for All; Brian Rosman, Research Director, Health Care for All; and Mark Benton, Program Officer, Milbank Memorial Fund.
The essays included in this collection do not always agree with one another, and they do not necessarily reflect the views of all members of the RSG. They all, however, represent the unique voice of states and amplify the critical role they play in our health care delivery system. All state leaders, particularly members of the RSG, look forward to collaborating with the federal government to develop a comprehensive approach to health care reform that will lead to healthier states and a healthier nation.
Carmen Hooker Odom
President
Milbank Memorial FundS. Peter Mills
Member, Health and Human Services Committee
Maine Senate
Co-Chair, RSG Steering CommitteeElizabeth Roberts
Lieutenant Governor
State of Rhode Island
Co-Chair, RSG Steering CommitteeCharles Scott
Chair, Labor, Health and Social Services Committee
Wyoming Senate
Co-Chair, RSG Steering Committee
Acknowledgments
The following people wrote essays and/or reviewed draft versions of the report. Their affiliation at the time of their participation is listed.
Martha B. Alexander, Co-Chair, Appropriations Committee, North Carolina House of Representatives; Thomas C. Alexander, Chair, General Committee, South Carolina Senate; Laurie Monnes Anderson, Chair, Health Policy and Public Affairs Committee, Oregon Senate; Holly Benson, Secretary, Florida Agency for Health Care Administration; Linda Berglin, Chair, Health and Human Services Budget Division, Minnesota Senate; Ned Calonge, Chief Medical Officer, Colorado Department of Public Health and Environment; Harriette L. Chandler, Assistant Vice-Chair, Senate Ways and Means Committee, Massachusetts Senate; Lawrence Clark, Director, Legislative Affairs, Pennsylvania Office of the Governor; Eileen L. Cody, Chair, Health Care and Wellness Committee, Washington House of Representatives; John Colmers, Secretary, Maryland Department of Health and Mental Hygiene; Kevin Concannon, Director, Iowa Department of Human Services; Gene Davis, Minority Whip, Utah Senate; Nile Dillmore, Ranking Minority Member, Insurance and Financial Institutions Committee, Kansas House of Representatives; Patricia Dillon, Assistant Majority Leader, Connecticut House of Representatives; Paul Dugdale, Director of Chronic Disease Management, Australian Capital Territory Health; Derek Feeley, Director, Healthcare Policy and Strategy, Scottish Government Health Directorates; Dede Feldman, Chair, Public Affairs Committee, New Mexico Senate; Jerry Fuller, Medicaid Director, Alaska Department of Health and Social Services; Eugene I. Gessow, Medicaid Director, Iowa Department of Human Services; Bruce Goldberg, Director, Oregon Department of Human Services; Richard N. Gottfried, Chair, Health Committee, New York State Assembly; Mary E. Grant, Member, Joint Public Health Committee, Massachusetts House of Representatives; Lee Greenfield, Senior Policy Advisor, Hennepin County Department of Human Services and Public Health; William D. Hacker, Commissioner, Kentucky Department of Public Health; Kemp Hannon, Chair, Health Committee, New York Senate; Toni Nathaniel Harp, Chair, Committee on Appropriations, Connecticut Senate; Jack Hatch, Chair, Health and Human Services Appropriations Subcommittee, Iowa Senate; David E. Heaton, Ranking Member, Health and Human Services Appropriations Subcommittee, Iowa House of Representatives; John A. Heaton, Member, Health and Government Affairs Committee, New Mexico House of Representatives; Nettie Hoge, Policy Director, California Office of the Lieutenant Governor; Thomas E. Huntley, Chair, Health Care and Human Services Finance Division, Minnesota House of Representatives; Karen Keiser, Chair, Health and Long-Term Care Committee, Washington Senate; Jane Kitchel, Vice-Chair, Appropriations Committee, Vermont Senate; Peter C. Knudson, Majority Leader, Utah Senate; Christopher F. Koller, Commissioner, Rhode Island Office of Health Insurance; Robyn Kruk, Secretary, Australian Government Department of the Environment, Water, Heritage and the Arts, and Vice-Chair, RSG Steering Committee; Scott Leitz, Assistant Commissioner, Minnesota Department of Health; Tony Lourey, Vice-Chair, State and Local Government Operations and Oversight Committee, Minnesota Senate; Angus MacIsaac, Minister of Economic Development, Province of Nova Scotia; Pam Maier, Chair, Health and Human Development Committee, Delaware House of Representatives; Steve Maier, Chair, Health Care Committee, Vermont House of Representatives; Anne L. McGihon, Chair, Health and Human Services Committee, Colorado House of Representatives; Rhonda M. Medows, Commissioner, Georgia Department of Community Health; S. Peter Mills, Member, Health and Human Services Committee, Maine Senate, and Co-Chair, RSG Steering Committee; Bob Nakagawa, Assistant Deputy Minister, Pharmaceutical Services, British Columbia Ministry of Health; Marcia J. Nielsen, Executive Director, Kansas Health Policy Authority; John T. Nilson, Member of the Legislative Assembly, Province of Saskatchewan; Scott Nishimoto, Vice-Chair, Health Committee, Hawaii House of Representatives; Alan Nunnelee, Chair, Appropriations Committee, Mississippi Senate; Suzanne Chun Oakland, Chair, Human Services Committee, Hawaii Senate; John M. O’Bannon, Member, Health, Welfare and Institutions Committee, Virginia General Assembly, and Vice-Chair, RSG Steering Committee; Gerry A. Oligmueller, State Budget Administrator, Nebraska Department of Administrative Services; Janet Olszewski, Director, Michigan Department of Community Health; Susan Paddack, Co-Chair, Appropriations Subcommittee on Education, Oklahoma Senate; Sheila Peterson, Director, Fiscal Management Division, North Dakota Office of Management and Budget; Sandy Praeger, Commissioner of Insurance for the State of Kansas, and Immediate Past President of the National Association of Insurance Commissioners; Sybil Richard, Deputy Secretary, Louisiana Department of Health and Hospitals; Elizabeth Roberts, Lieutenant Governor, State of Rhode Island, and Co-Chair, RSG Steering Committee; David Sater, Chair, Appropriations—Health, Mental Health and Social Services Committee, Missouri House of Representatives; Charles Scott, Chair, Labor, Health and Social Services Committee, Wyoming Senate, and Co-Chair RSG Steering Committee; John Selig, Director, Arkansas Department of Human Services, and Vice-Chair, RSG Steering Committee; Mike Shelton, Vice-Chair, Committee on Aerospace and Technology, Oklahoma House of Representatives; Betty Sims, Former Project Specialist, Missouri Department of Health and Senior Services; Joe Stegner, Assistant Majority Leader, Idaho Senate; Kathy Stein, Chair, Judiciary Committee, Kentucky House of Representatives; Leticia Van de Putte, Chair, Veteran Affairs and Military Instillations Committee, Texas Senate; Patricia Walrath, Co-Chair, Joint Committee on Health Care Financing, Massachusetts House of Representatives; Kevin Woods, Chief Executive, NHS Scotland, Director-General Health, Scottish Government Health Directorates.
Introduction
Every day, the U.S. health care system performs miracles for those in need of advanced and sophisticated medical services. It is justifiably regarded as the world’s leading research and technology development engine. And its workforce—though facing significant shortfalls in some professions—includes men and women with an extraordinary commitment to alleviate pain and ease suffering.
Yet, it is well-known that the U.S. health care system is falling short on three key dimensions of cost, quality, and access. President Obama and the new Congress have responded by placing health care reform high on the national priority list. State leaders look forward to working with the federal government to fashion a comprehensive approach to health care reform.
This essay collection, prepared by leading state health policymakers participating in the Reforming States Group (RSG), brings a unique state perspective to the health care reform debate. The essays included in this collection do not always agree with one another, and they do not necessarily reflect the views of all members of the RSG. They all, however, represent the unique voice of states and amplify the critical role states play in our health care delivery system.
In our federal system, most states have constitutional obligations to provide for the welfare of their citizens. State political leaders are accountable to their publics, even in the absence of federal activity in an area of need. States take this obligation seriously, both by initiating new programs and by filling in gaps of national endeavors. Secondly, states develop their own programs to meet their individual circumstances. As “laboratories of democracy,” states have valuable experience on which federal policymakers can draw. Moreover, states’ responsiveness to local needs often leads states to support some autonomy in fashioning programs that respond to their particular needs.
RSG BACKGROUND
The Reforming States Group (RSG) brings together leaders in health policy in the legislative and executive branches of government from the fifty states and several international jurisdictions to advance a state-federal partnership strategy for health care reform. As a bipartisan organization, the RSG recognizes the contribution states make in advancing a health care reform agenda, both by providing models for national efforts and by administering programs that reflect local needs. The impetus for the RSG came from activities in over a dozen states in the early 1990s when legislators and senior executive branch officials gathered to learn from one another and to press the federal government to implement health care reform programs.
With support from the Milbank Memorial Fund, the RSG prepared and distributed several papers during the Clinton-era health care reform debates. One notable report was Federalism in Health Reform: Views from the States That Could Not Wait, which detailed five principles for a successful state-federal health care reform partnership. These principles recognized the need for strong federal support that permitted flexible implementation and respected the states’ role as regulators of insurance. Though national health care reform was ultimately unsuccessful in the 1990s, the RSG was a prominent voice in those discussions.
Another notable example of the RSG’s influence was its contribution to the 1997 federal legislation that would become the State Children’s Health Insurance Program (SCHIP). A former member of the RSG, who was serving as staff director of the U.S. Senate Committee on Health, Education, Labor and Pensions, invited the RSG to help resolve a controversial issue in the House and Senate versions of the bills: the alternative benefit packages among which states could choose. In a letter to the members of the conference committee, the RSG recommended that the legislation permit states to choose one of four alternative benefit packages that RSG members had defined earlier in the year. The staff director later said the RSG’s intervention was “definitive” in enabling the conference committee to reach agreement on the final compromise bill. The final legislation included the four sets of benefits almost precisely as the RSG had formulated them.
The RSG has continued to work with state leaders on strengthening health care policy. RSG projects have looked at integrated health system regulation, health information policy, workforce concerns, children’s coverage, and prescription drugs (a list of RSG publications is included at the end of this report). A key concern throughout all of these endeavors has been federalism, finding an appropriate balance of state and federal responsibilities.
National health care reform should take advantage of states’ experience as providers and payers of coverage. Not only do states understand budgetary pressures as they are required to balance their own budgets, but also state lawmakers and officials are often much closer to the “problems on the ground,” enabling them to closely monitor and adjust policy to meet realities.
A new administration and a new Congress offer hope to states. Washington has the ability to be a partner with states: to facilitate program innovation, to fund programs that are cost prohibitive for states, and to set national standards to assure that all jurisdictions are on a level playing field.
States and the federal government must be partners in solving the current health care crisis. Heavy-handed federal action can stifle states’ ability to craft solutions that meet local needs, as well as impose needless costs and reporting requirements. However, like President Obama and the new Congress, states recognize that resolving our nation’s health care challenge is a necessary, critical component to overcoming our financial crisis. No longer can any of us support a health care system that is dictated by one’s ability to pay or one’s health condition. The time for action is now, not later.
STATE AND FEDERAL ROLES
States have been at the forefront of efforts to improve the health care system for much of the last two decades. A recent example is the Vermont Blueprint for Health Chronic Care Initiative that was launched in 2003 by Governor James Douglas and endorsed by the Vermont General Assembly in 2006. The initiative catalyzed a systems-based redesign of health care delivery focused on prevention and chronic illness as well as an expansion of coverage through the creation of the Catamount Health Plan. The systems transformation component has led to implementation of strategies to coordinate care; to expand use of medical information technology, including the development of a statewide health information exchange network plan; and to align fiscal incentives with health care goals. In Massachusetts, the landmark 2006 health care reform program—An Act Providing Access to Affordable, Quality, Accountable Health Care—guaranteed universal health insurance and was forged by then-Governor Mitt Romney and the overwhelmingly Democratic legislature, showing that a bipartisan consensus could be reached on universal health care coverage. The Massachusetts plan mixes sliding-scale subsidies to help low-income uninsured individuals enroll in coverage and provides incentives for both individuals and employers to participate in expanding coverage. After two years of implementation, more than 97 percent of Massachusetts residents have health insurance. Only 2.6 percent of state residents remain uninsured.
Earlier programs in Florida, Hawaii, Maine, Minnesota, Oregon, Tennessee, and other states have had varying degrees of success. Sustaining progress over time can be difficult as states are not as well-equipped as the federal government to ride the ups and downs of the economic cycle. Some states have proposed building in countercyclical funding structures that would automatically increase federal Medicaid payments during economic downturns. Other states are calling for a moratorium on all unfunded federal mandates.
In all of these programs, a productive state-federal partnership is a key building block. States depend on federal resources to pay for part of the cost of expanded coverage. Federal research findings through agencies like the Agency for Healthcare Research and Quality (AHRQ) provide critical support, such as best practices and measurement standards. Experiments allow states both to implement approaches that work best for their needs and to test new ideas that can show the way towards successful national health care reform.
FEDERALISM AND THE DIVERSITY OF STATE HEALTH SYSTEMS
An essential interaction is the relationship between state health policies and federal health policy—a cornerstone dynamic in all policy since the founding of the American republic. In health policy, federalism shapes Medicaid, insurance regulation, and a myriad of state rules that govern licensure and a scope of practice issues, food and drug policy, and much more.
States have distinct political and health system cultures, reflecting varying health care delivery systems and regulatory approaches. These differences show how local needs influence a particular state’s political system and health care marketplace. States vary in their rural and urban mix of populations, in their degree of competition among hospitals and health insurers, in their regulatory structures, and in many other dimensions. This variance creates state-specific health policy foundations that determine “rules of the road” for each state system. This diversity must be taken into account when designing federal policy.
Health policy must grapple with many crosscutting issues in our mixed system. Among these are the following:
- Diffuse payment structures: Health care costs have steadily increased faster than national income. States’ attempts to control costs by limiting payment amounts or reforming payment methodologies are challenged and influenced by the multiplicity of payers in our system. The federal government is the most conspicuous of these payers, accounting for around a fifth of all health care expenditures through its Medicare program alone. Medicare’s payment policy and benefits structure are set in Washington without regard to the interests of states. Without Medicare’s active participation, it is impossible for states to create uniform payment systems. The absence of such systems makes it difficult for states to implement payment incentives that promote effective utilization across all payers, such as adequate reimbursement for primary and preventive care that will, in turn, promote wellness and health.
- ERISA: The Employee Retirement Income Security Act of 1974 (ERISA) includes a side provision that prohibits states from regulating certain employee health benefits. While states can regulate insurers, most large employers self-insure and thus are beyond state regulation. ERISA serves an important federal goal, by facilitating interstate firms’ uniformity of benefit plans. However, it also interferes with states’ ability to control the largest single source of health coverage in any state. Many promising health reform ideas promoted by state legislators are preempted by ERISA and must be shelved.
- Regulatory variation: Among the states there is wide variation in required coverage. Some states have several dozen mandated benefits, while others have only a few. States’ insurance regulations also vary considerably. Several states prohibit insurers from taking into account an insured person’s health status, and many states without these “guaranteed issue” requirements have individual high-risk pools that may cover those who cannot obtain coverage from insurers. As a result, national insurers must change administrative procedures to comply with each state’s system. While states have primary responsibility for regulating insurers, the federal government enforces a number of mandates that overlay state requirements. HIPAA, COBRA, and other laws impact health insurance in specific circumstances. The most recent federal law, the Paul Wellstone and Pete Domenici Mental Health Parity and Addiction Equity Act of 2008, will broadly outlaw health insurance discrimination against Americans with mental health conditions and addictive disorders in employer-sponsored health plans.
- Practice variation: Comparisons of Medicare data show wide variations in practice across regions and localities. For example, in the last six months of life, the length of time patients may spend in a hospital or the number of doctors they see varies significantly by hospital region. People treated in one region spend an average of eight days in the hospital, while those in another spend thirty-five days. In one area, an average of fourteen doctors attend to a patient while in another area thirty-five doctors see a patient with a similar condition. The cost differential by region is more than a third higher. Moreover, patients in areas with more intensive and more expensive medical services often receive worse quality care than those with less intensive and less expensive care. Some states’ payment reform efforts are aimed at addressing some aspects of this particular problem. For example, states are requiring specific criteria for “dual eligibles” and special needs plans in contracts for Medicare and Medicaid.
- Population variation: States vary widely in their demographic makeup, economic bases, and social structures. A younger age demographic is relatively less expensive to cover than an older one. States with a larger proportion of low-wage workers have a much more difficult time paying for health care costs. Undocumented immigrants, who may pose both financial and service delivery burdens for states, will likely be a factor in any health care reform proposal.
As the new administration and new Congress begin consideration of comprehensive health care reform, the RSG offers these key recommendations:
- Rationalize financing through payment reform:
- Prioritize payments for primary and preventive care. Our current payment structure values intensive, specialty care, while paying much less for services designed to keep people healthy. Flipping these priorities will steer patients to cost-effective treatments that promote wellness and health. Equally important is to end Medicare’s regional reimbursement discrimination whereby states receive considerably more (or less) payment for the same procedure based upon geographic location.
- Implement coordinated systems of care. Medical homes are a practice format that emphasizes a coordinated focus on patient needs, with effective incentives for coordinated care among multi-specialties, especially in chronic care. Payment systems should promote integrated approaches that support coordinated care.
- Support value-based purchasing efforts. Value-based purchasing uses transparent quality and cost data and patient incentives to steer care towards high-quality, cost-effective providers. These methods have the promise to reduce cost and improve patient quality.
- Restructure national financing for long-term care. As baby boomers age, long-term care needs will skyrocket. A comprehensive financing strategy that takes into account states’ financial capabilities is critical.
- Guarantee access to affordable health insurance:
- Expand coverage to everyone. Using private market and publicly financed plans, affordable coverage must be guaranteed to every resident. The growing numbers of the uninsured impede economic opportunity and impact our national health. The United States must design a coverage system that leaves no one without access to affordable health insurance.
- Allow for greater flexibility in state regulation of ERISA insurance plans. The ERISA law precludes effective state oversight of self-insured employer-offered insurance coverage. This unintended consequence of ERISA distorts policy and interferes with a state’s ability to provide for consistency in coverage. Congress should carefully provide flexibility to states to require reasonable accountability on employer benefit plans.
- Eliminate “preexisting” conditions exemptions and require guaranteed issue of insurance. Permitting insurers to reject applicants based on health status leaves those who most need coverage without any affordable options, defeating the purpose of health insurance.
- Increase quality:
- Develop evidence-based standards for care that take into account clinical- and cost-comparative effectiveness findings. Care options should be weighed in terms of both effectiveness and price. Comparative effectiveness research that evaluates treatments in terms of efficacy and price will allow for the greatest value in health outcomes.
- Require the use of informed, shared decision making between provider and patient. Patients need to bring their preferences and values to the medical decision-making process, as providers bring their experience and knowledge of medicine. Informed joint decision making has been shown to improve outcomes and to increase patient/family satisfaction.
- Eliminate disparities and inequality in health care. Numerous social factors lead to widespread racial and ethnic disparities in health care. Our health care system needs to systematically address these disparities if our promise of health care for all is to be honored.
- Invest in effective prevention programs and health promotion activities. Public health activities such as promoting healthy behaviors and teaching disease management can improve overall health and lower costs. Government, schools, businesses, and community groups all can play a role in patient education for health.
- Reduce unwarranted variation in care. There is substantial evidence showing that wide variations in care, either overuse or underuse of certain treatments and services, adversely impact health outcomes and spending. Evidence-based practice guidelines reinforced by a payment system that encourages care proven effective will optimize practice patterns to improve health and avoid needless costs.
- Require public quality reporting by all providers on state and national quality measures. Reporting allows consumers to choose high-quality providers and thus spurs providers to improve care. Measures must be understandable to the public and provide valid comparisons based on reliable data.
- Create national standards for health information technology interfacing and interoperability:
- Provide financial and technical assistance for the adoption of electronic medical records. Modernizing medical records using current technology will improve care and lower costs. Patients must be assured of privacy protections and be permitted to access their own data. A universal system of medical records will reduce system waste, improve care quality, and lower system costs.
- Facilitate the sharing of data within and across state borders. National inter-operational standards will allow providers to access patient records anywhere. Strong federal leadership is required to set national standards and create a technology infrastructure that allows records to be accessed by all of a patient’s caregivers.
- Build an appropriate health care workforce:
- Invest in increasing the number of primary care providers, midlevel practitioners, direct care workers, laboratory and community health workers. These professionals are in short supply and offer the most value by providing primary care and preventive services. The federal and state governments should explore ways in which federal and state payments, such as Teaching Disproportionate Share Hospital (Teaching DSH), Indirect Medical Education (IME), and Graduate Medical Education (GME), could be used to influence and increase the number of physicians specializing in primary care and other hard-to-recruit disciplines. Providers, businesses, and members of the labor and the academic community must collaborate to provide incentives for addressing the workforce needs of the coming decades.
- Carefully monitor specialty supply. Certain specialists are in overabundance, and policymakers need to be attentive to these circumstances.
ABOUT THIS PUBLICATION: ESSAYS FOR THE NEW ADMINISTRATION AND CONGRESS
The inauguration of the new federal administration and Congress provides an opportunity to reflect on the past in order to inform and guide the future. Collectively, members of the RSG in legislatures, secretariats, commissions, and agencies bring hundreds of years of policymaking experience and wisdom to this task. From insurance regulation to Medicaid administration, from public health to long-term care, RSG members have wrestled with high levels of complexity and uncertainty.
RSG members volunteered to write essays to be included in this report on topics of particular relevance and importance. The essays reflect the individual ideas and preferences of the authors, who span the ideological and partisan spectrum. The essays address the following topics:
The RSG offers these essays as a guide to the new administration and Congress for health care reform from the states’ perspective. They also provide a useful overview of health policy topics for the public. As we embark on a national dialogue that hopefully will lead to a healthier America, the RSG urges federal policymakers to carefully heed the voices from the states.
Access to Care
For nearly two decades, a number of states around the country have engaged in health care reform initiatives. These efforts have largely focused on expanding coverage within the context of federal Medicaid waiver authority as the way to increase access to care. However, coverage by itself does not provide access to the right care at the right time, particularly for individuals with chronic illness. In addition, the unrelenting increases in health care costs pose a constant threat to these state efforts.
The time has come for reform to be undertaken in a much broader fashion. The economics speak for themselves. Costs that exceed income and revenue growth year after year cannot be sustained indefinitely. One has only to look at the TennCare program where thousands of individuals lost coverage and access to care because of unsustainable costs. Less draconian cost reduction strategies frequently used by states include increased cost sharing by beneficiaries, limiting benefits, capping enrollment, and shifting costs from public programs to other payers.
No state by itself can undertake a comprehensive health care reform effort that controls costs, improves care, pays for population health, and provides universal coverage. Sustainable reform requires a strong federal-state partnership and the involvement of all major insurers. Medicare and Medicaid must be involved in any systems-based changes that include financial reform, clinical transformation, a focus on prevention, and a statewide health information infrastructure. Currently, there is no mechanism for Medicare to participate in state-initiated health care reform. This is essential. The federal government must be a full partner and establish a flexible mechanism for Medicare to participate in innovative state-led initiatives.
Considerable attention is inevitably being given to individuals with chronic illness since estimates suggest that 75 percent of total health care spending is driven by care provided to these individuals. A traditional approach used by insurers to control the cost of care has been to overlay a disease management program using claims data. This is often not well-received by providers who feel second-guessed or by patients who tire of mealtime phone calls from out-of-state nurses. Most importantly, it is duplicative, reactive, and symptomatic of the shortcomings of a system that was designed to provide acute care—not chronic care.
Under our current delivery system, studies have found that only about 50 percent of patients receive recommended preventive care and 60 percent receive recommended chronic care. These data provide a compelling case for the need to reengineer the delivery system as part of any health care reform efforts to achieve access to appropriate care. Mechanisms that assure the delivery of the right care at the right time must be built into the system. This restructured delivery system will require robust IT support so that independent primary care physicians and midlevel practices have access to electronic medical records and are connected to a statewide health information exchange network. This level of IT infrastructure will necessitate significant public funding.
Vermont provides an example of how an IT infrastructure can be integrated into a health care delivery system. To provide the organizational leadership and capacity required to plan and develop a statewide health information infrastructure critical to health care reform, Vermont created a public-private partnership named Vermont Information Technology Leaders (VITL). This organization is “charged with developing Vermont’s statewide, integrated, electronic health information infrastructure for the sharing of health information among health care facilities, health care professionals, public and private payers, and patients.”
To date, VITL has implemented a medication history service in three hospitals and electronic health records (EHRs) in five small primary practices, and is addressing the thorny issues of privacy, security, and patient consent.
In the 2008 session, the Vermont legislature tackled the financing for this statewide health information infrastructure by imposing an assessment on all insurance claims and dedicating these revenues to the Health Care Information Technology Fund. Grants will be made from this fund to primary care practices to subsidize the cost of EHR procurement and implementation. This fund will also pay for the Health Information Exchange Connectivity Service between hospitals and other providers. These efforts will be rolled out over a period of seven years before the statewide infrastructure is complete.
Any restructuring of the delivery system must be accompanied by a reform of the existing payment system. Chronic care management systems that are viewed as effective build on the concept of a “medical home.” Providing medical homes requires sufficient primary care capacity and changes in reimbursement for primary care services, which are often not covered or not adequately reimbursed for the time required.
Vermont, an early participant in health care reform efforts, has moved to the next phase of reform with the development and implementation of a model for prevention and care called the Blueprint for Health. This model, as displayed in the diagram below, addresses the full continuum of health care reform components. After many years of focusing primarily on coverage expansions, Vermont has broadened the scope of public policy development and legislation to encompass the full continuum of reform elements.
The diagram illustrates the interconnected nature of the various reforms that are essential to comprehensive health care reform. The nested ovals at the top illustrate three areas for change, which must act in concert to produce results. On the outside, encompassing the entire system, is public health, particularly increased focus on prevention efforts and support for community infrastructure that fosters physical activity. For example, the Vermont plan includes a five-year Vermont Pedestrian and Bicycle Policy Plan, integrated with the Fit and Healthy Vermonters advisory committee. The Blueprint recognizes that public health interventions can be the most cost-effective means of improving overall health.
Community resources are encompassed by the public health area. A key initiative here stresses chronic disease self-management. This paradigm emphasizes the role individuals can play in managing their own health. Workshops being held throughout the state teach proven methods that empower people with chronic diseases to keep themselves healthy. The techniques provide tools for patients to manage medications, reduce pain and fatigue, and eat healthier. They have been shown to increase energy, build self-confidence, and reduce medical costs.
Finally, within each of these fields are improvements to the health care delivery system. Web-based patient information systems, clinical treatment guidelines and best practices, and outcomes measurement enable physicians and other medical providers to focus on proven cost-effective chronic care treatments.
These factors combine to produce a supportive environment that aligns patients and practitioners to improve health and reduce costs. The hoped-for outcome—a healthier population—can be achieved if all parts of the system are pulling in the same direction.
Costs that do not contribute to improved health outcomes must be identified and stripped out of the system. Examples of administrative streamlining include policies such as single credentialing of providers for all payers and the use of common claims forms and consistent care protocols across all payers, both public and private. This will require all payers to work together in a more consensus-driven fashion than has historically been the case. Likewise, on the care delivery side, where estimates suggest that 20 to 30 percent of health care spending goes for unnecessary care, we must expand and develop the capacity to undertake systematic reviews of specific treatment modalities. A notable example of such an effort is Washington’s Health Technology Assessment (HTA) program.
Like Washington’s program, any national or state initiative must be a data- and evidence-driven process that helps identify procedures that should not be covered because of a lack of demonstrated medical efficacy or because there is a less costly intervention that produces equally good results. Without this capacity, there is no organized method to counter the marketing efforts of the drug and equipment manufacturers.
As a nation we should be very concerned about the rapidly increasing prevalence of chronic illnesses, particularly diabetes, high cholesterol, and heart disease, and the extent to which these illnesses are attributable to obesity. In a 2004 article in Health Affairs, Kenneth Thorpe and colleagues studied the impact of obesity on health care spending and estimated that the “increases in the proportion of and spending on obese people relative to people of normal weight account for 27 percent of the rise in inflation-adjusted per capita spending between 1987 and 2001.” Nothing is more effective in controlling costs than disease prevention and avoiding unnecessary treatment. Our public health infrastructure and expertise are uniquely positioned to lead the needed preventive and health promotion initiatives that can help improve the health status of Americans.
Keys to achieving access to the right care at the right time include the following:
There is much critical work ahead as states continue their health care reform efforts. As John Muir, the great conservationist, said, everything is “hitched to everything else.” Successful and sustainable efforts to expand coverage and access to health care must be “hitched” to a comprehensive reform approach that includes cost containment, health promotion and disease prevention, changes in the delivery and payment systems, and involved and knowledgeable consumers. To focus on coverage alone runs the risk that these efforts will be akin to Sisyphus pushing the proverbial boulder up the hill.
Jane Kitchel, Vice-Chair, Appropriations Committee, Vermont Senate
Controlling the Cost of Care
Managing the cost of health care, a cost escalating at a rate far in excess of broader economic trends, must be a major component of health care reform. Whether looking at public programs like Medicare or Medicaid or the challenge of maintaining individual and employer-based commercial insurance, managing costs is crucial. The many efforts to expand coverage will be unaffordable, and the number of employers providing health insurance will continue to decline if there are not effective approaches to managing the cost of medical care in the United States. Such approaches must cross public and private programs and require better cost and utilization trends and improved health behaviors that lower the lifetime cost of care for all of us. As chronic disease accounts for over 75 percent of health expenditures, a focus on prevention of chronic disease and on effective management of diagnosed chronic disease is crucial.
Administrative efficiencies that lessen duplication of services and minimize staff needs for billing and utilization review should be accomplished as quickly as possible through the effective integration of information technology across health care settings. For example, Utah and other states have promulgated rules for uniform claim forms and billing codes and compatible electronic data interchange standards. If savings of up to 30 percent can be achieved through national IT adoption, then we must make this investment. It will also significantly enhance the quality of care we all receive.
Administrative changes alone, however, will not solve our biggest cost challenges. One of the most important steps in managing cost effectively is to integrate reforms in the public and private sectors. Imposing a Medicare reimbursement cut while ignoring the implications of that cut, such as cost shifting to other payers, is shortsighted. Payment reform that uses capitation, bundled payments for episodes of care, and other payment mechanisms to improve quality and effectively manage utilization should be implemented in public and commercial programs. Hospitals and physician practices both should be impacted by payment reform. Ancillary health care providers, who are often more cost-effective but least able to succeed financially in the current reimbursement system, should be integrated into a broader system that pays for effective disease prevention and management.
None of the shifts in focus and reimbursement should mean that people do not have access to care, especially specialty care, when needed. However, supply of those services should be allocated to meet the needs of the population. Rapid escalation of costs, particularly for specialty testing and new technology, should be slowed through a renewed certificate of need process that works. The past two decades have shown that proliferation of specialty services has increased costs without necessarily improving health.
Aligning financial incentives to the needs of the community rather than to the economic imperatives of the health care industry is necessary to control cost growth. Our current system rewards expensive specialty care and high-tech diagnostic procedures more than primary and preventive care. This imbalance of incentives drives costs ever higher. Also, as demographic changes cause our population to be older with greater health needs, costs will escalate much more rapidly. Just as we should implement public and private payment reforms, we should also integrate health policy changes in the long-term care and acute care delivery systems. The divide in how policymakers view these two parts of the health care delivery system and the echoing difficulty consumers have in using services effectively during a long-term illness have led to expensive inefficiencies.
Delivery and payment system reforms can only be part of managing health care costs. Maintaining a focus on childhood and adult immunizations, clean water and air, and other population health investments will continue to lower health care needs. Recognizing the cost implications of poor health behaviors, such as eating unhealthy foods, smoking, and failing to exercise, must also stay at the top of our health care reform agenda. For example, Vermont’s Catamount program emphasizes statewide education on healthy behaviors and good nutrition. Federal support for such state efforts could pay off in reduced Medicare and other costs down the line. Simply adjusting payment mechanisms without having us work to improve our own health will be inadequate to meet the cost of health care.
A successful cost control strategy must incorporate five key activities: (1) coordinate cost management strategies across public and private programs alike; (2) promote administrative efficiencies; (3) examine effective certificate of need programs to determine their impact on the proliferation of new technologies and specialty services; (4) integrate health policy changes in both the long-term care and the acute care delivery systems; and (5) invest in prevention and comprehensive public health initiatives.
Elizabeth Roberts, Lieutenant Governor, State of Rhode Island
Controlling the Cost of Care
Controlling the rate of increase of medical costs is an essential part of any health coverage reform. Since the mid-1990s, health care spending has grown much more quickly than national income. For any reform plan to be viable over the long term, the rate of increase in health care costs has to roughly match the real growth rate of the economy, as governmental revenues will generally grow at these rates.
There are many opportunities for cost control. This essay will focus on three important methods: reducing medically unnecessary care, reducing prescription drug costs, and reducing administrative costs.
I do not include reducing provider reimbursements or rationing needed care as those strategies are counterproductive. While American provider reimbursements are high, our
free labor market requires that highly skilled professional labor be well paid. A typical government cost control strategy has been to hold down public reimbursement rates and induce providers to cost shift to the private sector. In Wyoming, we figure that governmental cost
shifting increases private pay hospital costs by 20 percent. This inequitable strategy just leads to growing private health insurance costs, particularly as the government’s share of health care payment grows.
While we need to accept high reimbursement rates, adjustments in relative reimbursement rates should be made. Primary care reimbursement should increase relative to specialist reimbursement, but this is unlikely to reduce total spending.
Rationing should not be used as a strategy because it is both unnecessary and immoral to ration needed care when we are paying for so much unneeded care. While it is tempting for a health care reform plan to prohibit unnecessary care, this strategy is unlikely to be successful. First, the providers whose income is being limited put their congressmen or state legislators on speed dial and bring enough pressure to stop controls. Second, outright bans don’t recognize that procedures can be appropriate in some circumstances and wasteful in others. A top-down, command- and control-oriented governmental bureaucracy has trouble distinguishing between unnecessary and legitimate procedures.
In any case, we are already paying for a great deal of unneeded care. The Dartmouth Atlas Project, led by Doctors Elliot Fisher and John Wennberg, estimates that up to 30 percent of our medical spending for chronic care (which accounts for 75 percent of all health spending) is unnecessary. In my view, there are three main causes of this overuse:
Market solutions can be used to reduce prescription drug costs. For most pharmaceutical needs there are multiple drugs, both generic and brand name, offered at competing prices. Pharmacists, who do not have a financial interest in selling patients a particular drug, can advise patients on both safe substitutions and relative prices. In Wyoming, the state government offered consultations to people using multiple prescription drugs. Their average savings from substitutions and from discontinuing unneeded drugs was $2,000 per year.
There are a number of opportunities to save administrative costs. Electronic billing and reimbursement systems have already been implemented, at least in part. Electronic medical records (EMRs) have promise, but I don’t think we can yet say they will reduce costs as opposed to improving quality without increasing costs. While a single payer system would reduce administrative costs, its many problems are beyond the scope of this essay.
I have proposed a package of insurance reforms for low-income uninsured people in Wyoming with four elements:
Through these steps, we can reduce the skyrocketing cost of medical care and lower the price paid by government and individuals in providing coverage.
Charles Scott, Chair, Labor, Health and Social Services Committee, Wyoming Senate
Quality of Care
Despite spending substantially more per capita for health care than any other country in the world, the United States, by most objective measures of quality, lags the rest of the developed world. While this disparity in cost and outcomes has been known to policymakers for years, there is a widespread perception by the public, fostered by many in the health care field, that our health care system is the envy of the world. While a portion of the population has nearly immediate access to all the advances of modern medical technology, it has become increasingly clear, even to those with such access, that the health and medical care systems are not delivering the outcomes they could, resulting in underuse, overuse, and misuse of resources.
The clarion call for change began with two seminal Institute of Medicine reports—To Err is Human (2000) and Crossing the Quality Chasm (2001)—which highlighted first the problems with patient safety and more broadly the failings of quality along other important dimensions, including care that is effective, patient-centered, timely, efficient, equitable, integrated, and affordable.
The states have long been at the forefront of the quality movement. Numerous states have developed and published report cards on payers’ and providers’ performance well before the Medicare program published its Nursing Home Compare and Hospital Compare websites. For example, in Minnesota, the Institute for Clinical Systems Improvement brought together fifty-six medical groups and six health plans to develop best practice health care guidelines for the prevention, diagnosis, and treatment of health conditions. Their work supports public quality reporting to help patients make informed choices. Similarly, several states have taken the lead in publicly reporting “never events” and establishing payment systems that provide both rewards and penalties to providers based on performance. Several states have recently established collaborative approaches involving providers and payers to improve outcomes in the detection and treatment of chronic diseases.
Despite these advances, policymakers continue to face significant challenges to improving the performance of the health and medical systems in their jurisdictions. Among the many obstacles are the following: (1) there is a lack of electronic medical records and related information systems that support collaborative decision making; (2) there are significant and intolerable differences in health outcomes for various racial, ethnic, geographic, and socioeconomic groups that persist even among groups with comparable insurance coverage—underlying these variations are provider practice patterns and cultural insensitivities that are resistant to change; (3) the medical liability system in most jurisdictions creates barriers to transparency and is used to support unnecessary defensive practices; and (4) payment systems for physicians and hospitals remain disjointed and dominated by a Medicare system that remains beyond the reach of state policymakers. Because Medicare generally pays providers on a fee-for-service basis, with few quality incentives, Medicare’s rules often become default practice standards for many doctors and hospitals.
There are a number of steps federal policymakers can take to accelerate improvements in our health care system:
John Colmers, Secretary, Maryland Department of Health and Mental Hygiene, and Pam Maier, Chair, Health and Human Development Committee, Delaware House of Representatives
States and the Employee Retirement Income Security Act (ERISA)
The highest mission of American federalism, its greatest strength, arises from our shared capacity to experiment among the states, so often referred to as our “fifty laboratories of democracy.”
All governments make mistakes. Big governments make big mistakes. The virtue of our federal system is states’ capacity to solve problems in different modes and at smaller scale, to gather evidence about what works, and to foster sound solutions for our nation as a whole.
American health care, at a cost of two trillion dollars a year—equal to 16 percent of GDP—is by far the largest, most complex, and most broadly deficient system under discussion in the nation today. No one from any sector of the political spectrum is content with its present function. It compares unfavorably with health care in nearly every other developed nation in terms of cost, coverage, efficiency, and end result.
Yet our states are hamstrung. In the field of health care, the states have been denied for thirty-five years their inherent capacity for initiative because of a few words in a law called ERISA—the Employee Retirement Income Security Act of 1974.
Envision for a moment how much we might learn if a state had power merely to aggregate in a pilot program all the medical costs in just one county and redeploy those dollars to maximize the health of every citizen in the region. As tempting as such a civil experiment might be, ERISA renders it impossible.
ERISA by its own terms “supersede[s] any and all State laws insofar as they may . . . relate to any employee benefit plan” covered by the act. By these words, Congress has preempted, or nullified, all state laws relating to health benefit plans sponsored by a self-insured employer. Although there is a “savings clause” to acknowledge that regulating insurance remains the
province of the states, states may not “deem” or treat as insurance any benefit plans within ERISA’s broad ambit.
ERISA’s practical effect is to leave a large segment of the private coverage market devoid of effective regulation. Aggrieved consumers under ERISA plans are turned away by state agencies and referred to distant federal offices of the Department of Labor with few protections to offer. States have tried through federal courts to discern the contours of what ERISA permits and forbids, but the costly litigation has resulted in division, shifting standards, and uncertainty.
The Reforming States Group suggests a more balanced approach, one that will recognize a mutuality of interest at both levels of government. We offer the following as examples of how state and federal relations under ERISA might be improved:
S. Peter Mills, Member, Health and Human Services Committee, Maine Senate, and John Colmers, Secretary, Maryland Department of Health and Mental Hygiene
Insurance Market Reform
Both at the federal and state levels, the goal of most health insurance reform efforts has been to enhance access to affordable, sufficient coverage. Various guaranteed issue requirements, rating reforms, benefit mandates, and other reforms have been implemented. More comprehensive reform will require federal-state coordination and cost management to be effective and must be informed by state experiences because all reforms have significant consequences—both positive and negative.
States have implemented health insurance reforms to meet the specific needs of residents and to reflect market realities. For example, New York recognized that insurance was unaffordable for most low-income individuals in its reformed marketplace, so the state implemented Healthy NY, a reinsurance-based reform, to provide more affordable options. Wisconsin and Idaho creatively use high-risk pools to address individual market access and affordability issues although segregating high-risk individuals in a separate pool makes it cost prohibitive to cover more than a small fraction of the uninsured in this manner.
Massachusetts has combined the individual and small group markets in one pool, with guaranteed issue and a “personal responsibility” mandate to spread the costs of high-risk individuals across a much broader risk pool. Massachusetts’s reforms, which also include the Commonwealth Health Insurance Connector, demonstrate that states can be laboratories for testing new ideas but also suggest that federal policymakers be wary of “one-size-fits-all” solutions.
State reforms often focus on the small group market because this market does not have the same advantages of pooling and spreading of risk that are inherent in large groups. Premiums for small employers are more volatile because even one sick worker can greatly increase costs. To address this issue, states have required guarantee issue (also a federal requirement) and instituted community rate, adjusted community rate, or rating band systems that eliminate or limit the ability of insurers to price risk based on health status and other factors. Of course, such reforms can significantly impact the composition of the pool. Rating reforms must carefully consider the risk population and the marketplace.
In some states, the individual market has grown and become a priority. A few states require guarantee issue of coverage and some have applied community rates. However, these reforms tend to raise costs, at least in the absence of a Massachusetts’s style individual mandate, so most states still allow insurers to deny or price coverage in the individual market based on health status.
Federal law can help or hurt state efforts. The Health Insurance Portability and
Accountability Act of 1996 (HIPAA), for example, is built on state reforms and provides important consumer protections. On the other hand, ERISA prohibits state oversight of self-insured plans, even though those plans impose burdens on employees, health care providers, and public aid programs. State regulators support more data from these plans, more protections for their enrollees, and more flexibility to encourage employer-based coverage through “pay or play” programs that reward employers that provide their employees health insurance coverage. All of these reforms can be accomplished without compromising the multistate nature of these plans.
Federal health care reforms must not focus only on allocation of costs—they must also confront the fact that those costs are escalating. Again, states lead the way. States are implementing reforms to address chronic conditions and frequent comorbidities. States like Vermont have instituted strict mental health parity requirements. Other state-based programs are developing best practices for treatment of chronic conditions, compensating providers that adhere to those protocols, and investing in medical records technology. Policymakers must continue to monitor these types of programs and encourage effective reforms.
State insurance regulators strongly support health care reform. Meaningful action is overdue. We encourage federal policymakers to work with states and rely upon states’ experiences. Together, we can implement reforms that will protect and assist all consumers.
Sandy Praeger, Commissioner of Insurance for the State of Kansas, and Immediate Past President of the National Association of Insurance Commissioners
Long-Term Care
While some 47 million Americans lack health insurance, 240 million Americans are uninsured for long-term care. This situation has the potential to create significant problems in the years ahead as a growing and aging population puts increasing strain on system capacity and financial resources.
According to the Urban Institute, even under the most optimistic disability scenario, which assumes that disability rates fall by 1 percent per year, the size of the disabled older population will grow by more than 50 percent between 2000 and 2040. Joining this group as major users of the long-term care system are individuals under age sixty-five with a disability.
The potential costs are significant. In 2005 Medicaid spending for long-term care totaled $94.5 billion—31 percent of all Medicaid expenditures. Of this amount, 63 percent was spent on institutional care and 37 percent on noninstitutional care. While institutional care is generally the more expensive of the two options, most consumers prefer to receive long-term care in their homes and communities. However, premature admission to and overuse of nursing homes are common.
The crucial challenges facing our nation’s long-term care system remain ensuring sustainable financing, a skilled long-term care workforce, and the availability of quality services. Arkansas was the first state in the nation to offer Medicaid consumers an opportunity to exchange a Medicaid service for a cash allowance and assume the responsibility of arranging for the services they need and desire. The program, called IndependentChoices, allows family members or friends to become paid personal care assistants—thus, substantially increasing the pool of workers, particularly in rural areas where there is a shortage of in-home care workers. Data from an independent evaluation indicated that consumers who directed their own care were less likely to use nursing homes and hospitals than their counterparts who received in-home care from an agency.
Providing access to affordable long-term care through a supplemental long-term benefit (within Medicare or other funding mechanisms) and assuring that long-term care issues are addressed as part of any national health care reform effort will be critical components of any national solution. In addition, there is general agreement among Congress, governors, and advocates that the long-term care system needs to be “rebalanced” to address the larger systemic issues. This can be achieved through the following actions:
And at the national level, the federal government can help rebalance the long-term care system through the following actions:
John Selig, Director, Arkansas Department of Human Services, and Bruce Goldberg, Director, Oregon Department of Human Services
Mental Health and Addictive Disorders
Mental illness and addictive disorders are two significant issues facing state policymakers today. That’s because states are struggling to meet staffing demands for psychiatrists and other mental health and addiction professionals who are both adequately trained and willing to work in the public sector (particularly those who are willing to treat children). An aging workforce with limited strategic focus on developing and targeting career paths in the fields of mental health and addiction treatment compounds the problem. Further, geographic barriers related to a largely rural landscape for the state of Louisiana dictate needed expansion of funding for the development of community-based treatment services.
The federal government must take the lead in raising awareness of mental health and addictive disorders and bringing both to the forefront of the U.S. health care system. The recent passage of the federal legislation on mental health and addiction parity was an important step in that direction. Congress and the former administration should be commended for it as this much-needed action will likely provide an estimated 100+ million people with access to insurance coverage. However, it still does not move this country close enough to recognizing mental health and addictive disorders on the same level as primary care, nor does it address the substantial number of uninsured who will not benefit from the legislation.
Every day, citizens from all fifty states die from mental illness and/or addictive disorders. One reason is because people with mental illness and addictive disorders—particularly those with chronic, severe functional impairment—do not seek treatment, nor do they take care of their physical health needs. Some of those who want to seek treatment often cannot, citing a shortage of providers, the presence of a waiting list, a lack of health insurance, or insufficient funding as the chief culprits. These uncertain economic times make it imperative that treatment for mental health and addictive disorders is adequately funded at both the state and federal levels.
A handful of states are turning to integrated care in hopes of improving the health care outcomes for people with mental illness and addictive disorders. Early signs show that this approach is working. In an integrated care environment, primary care doctors and behavioral health (mental and addictive disorders) practitioners collaborate on the care and treatment of the “whole individual.” Some models incorporate co-location of staff, disease management techniques, and case management services. In Louisiana and Utah, state agencies are working to implement a full medical home model that includes primary care, behavioral health care, and disease management.
Funding to support integrated care models and the larger array of behavior health care services is a huge problem for states as the demand for services far outpaces our ability to pay. Federal funding is also “siloed” and often tied to a categorical funding stream. Clearly, more flexibility in federal funding is needed—perhaps even allowing a handful of interested states to pilot and pursue a mental health “block grant.” Also, eligibility for federal programs/reimbursement should reward, not punish, people with mental illness and addictive disorders for pursuing work. Expansion of mental health and drug courts is needed in addition to increased education and collaboration with the criminal justice system. And best practices should be explored, particularly
for treating the incarcerated who have addictive disorders. In fact, Utah and Louisiana are strengthening their mental health systems to include assistance with employment and housing as they have found that individuals do better when they work and have a home. Federal policy and funding should follow their lead.
Hurricanes Katrina and Rita pulled back the curtain on the system of mental health and addictive disorders treatment in the United States. This national tragedy highlighted the fact
that all jurisdictions must have access to emergency behavioral health services, evidence-based
and community-based treatments, and a sufficient supply of mental health and addiction professionals, as well as adequate housing for people with severe mental illness and co-occurring addictive disorders.
The federal government can serve a vital role in the identification, dissemination, and support of best and evidence-based practices. In fact, many states have looked to the Substance Abuse and Mental Health Services Administration (SAMHSA) for such guidance; however, its sister agency the Centers for Medicare and Medicaid Services (CMS) routinely rejects coverage for newer and more cost-effective treatment models, which are proven best practices. It is all too common for states to find themselves in the untenable situation whereby SAMHSA is encouraging—if not requiring—them to implement a particular behavioral health service/approach, and CMS is refusing to fund it under the state’s Medicaid Plan. A key task for the new administration is to stop this practice. The two agencies must be required to work more collaboratively and to ensure that their policies and regulations support and complement one another. Rescinding the proposed regulations on school-based administration, case management, and the rehabilitation option are critical first steps to take in the right direction.
Gene Davis, Minority Whip, Utah Senate, and Sybil Richard, Deputy Secretary, Louisiana Department of Health and Hospitals
Public Health
In the early twentieth century, long before antibiotics and health insurance, Hermann Biggs, New York’s first state health commissioner, said: “Public health is purchasable. Within a few natural and important limitations any community can determine its own health.” The Institute of Medicine defined the mission of public health “as fulfilling society’s interest in assuring conditions in which people can be healthy.”
“Public health” is often thought of in terms of agencies providing local “safety net” clinical services. However, the scope of public health responsibilities is much broader. While some variation occurs between states, most public health agencies are responsible for promoting population health activities (for example, diet and exercise), protecting the public from threats (for example, emergency preparedness), and preventing outbreaks of disease (for example, immunizations). Furthermore, “public health” is a local, state, federal, and global enterprise system in which the local health department is directly connected to the state department for public health, which in turn is connected to the Centers for Disease Control and Prevention, which likewise is connected to the World Health Organization. In today’s world, a thread connecting a rural community in Wyoming to citizens in Cambodia occurs in real time and represents constantly moving people and risks in multiple directions.
Public health today deals with daunting challenges:
Furthermore, frequent international travel, common importation of food and consumer products (for example, toys), and the constant threat of emerging infectious diseases (for example, multiple-drug-resistant tuberculosis) require every community, both rural and urban, to think globally while acting locally.
Emergency preparedness is a growing public health focus, including preparing to respond to disease outbreaks or epidemics, injuries and illness caused by natural or human-caused disasters, and disruptions of health systems and services by disasters. Under Emergency Support Function #8—Health and Medical Services, the federal government requires state, local, and tribal public health agencies to be responsible for providing or assuring the provision of critical health and medical services during times of an emergency. This is an important expansion of the role of public health since the fall of 2001. Recent weather-related events have demonstrated public health’s important contributions under this new emergency response mandate.
Public health is overwhelmingly a state and local responsibility in the United States. Infectious diseases are reported to state or local health departments, and the people who work there are the
ones who inspect restaurants and conduct contact notification for sexually transmitted infections. When birds started dying mysteriously, it was a New York state health department laboratory scientist who discovered they were dying of West Nile virus.
Public health is very labor-intensive, and the people who pound the streets and work in the laboratories are predominantly state and local civil service professionals.
There also is and long has been a major federal role in public health. From the early days of the country, federal authorities have helped protect our borders and shores from infectious diseases. The surgeon general’s agency is the U.S. Public Health Service. The Centers for Disease Control and Prevention (CDC) and the Health Resources and Services Administration (HRSA) do indispensable work for the country and for state and local public health agencies. We all rely on CDC and HRSA programs and guidelines in a host of areas. The U.S. Food and Drug Administration is also a key part of the public health system. This structure has served the United States well and should be preserved.
State and local public health services, like many other services, have benefitted from federal financial support, through a variety of targeted grant programs such as the Ryan White HIV/AIDS Program. Such programs should be strengthened; specifically, the federal government should expand the resources for and strongly support state and local decision making and service delivery.
New York State provides state matching funds to support a broad range of local public health activities. The federal government should seriously consider a similar program of broad flexible public health funding to the states.
Remember that public health is purchasable and that government at every level shares responsibility for fulfilling society’s interest in assuring the conditions in which people can
be healthy.
Richard N. Gottfried, Chair, Health Committee, New York State Assembly, and S. Peter Mills, Member, Health and Human Services Committee, Maine Senate
Workforce Development
There have been much dialogue and some state and local action on health care reform, but this is now widely recognized as a priority issue for all Americans. Costs are high, insurance coverage is nonexistent or inadequate, and quality of services vary, all of which have led to a long discussion over whom and what our health care coverage system should and should not cover. A core problem of the high costs and varying quality of health care in the United States is a shortage in a quality health care workforce. Even if we can figure out the details of who is covered or not covered by our plans and of how to control spiraling costs, these details will offer little to no value to Americans if we do not address the shortages and quality of our future health care workforce.
The United States is facing a shortage of health care professionals, including primary care physicians and physicians working in underserved areas. In Texas, our inadequate supply of physicians is exacerbated by the fact that they are also disproportionately located in large urban areas. Our retiring baby boom generation of physicians will add to the increase in demand from all the retiring baby boomers. Sadly, we continue to perpetuate barriers that do not allow our health care system to grow and thrive. One of those barriers is the cost of attending medical school when the average public medical school debt is over $100,000. Over the past twenty years, the number of Texas medical school graduates has remained relatively flat but our population has grown by 50 percent in the same time span.
A severe underrepresentation of Hispanics and African Americans in our health care workforce complicates this problem. Texas demographic projections indicate that in thirty years the state will have a greatly increased number of economically, socially, and academically disadvantaged students. Therefore, we have implemented programs that encourage students to enter the health care workforce and provide support for them to successfully do so. We have implemented stronger career and technology funding to provide students in the early grades with the opportunity to experience various medical careers while they obtain college credit. This “medical careers pipeline” is facilitated at the higher education level with programs such as our Joint Admission Medical Program (JAMP).
The best predictor of where a doctor will eventually practice is where the doctor considers home. Therefore, to increase the number of physicians in areas that currently are medically underserved, the JAMP program focuses on providing services to support and encourage highly qualified, economically disadvantaged students pursuing medical education. Recruiting students from rural and inner-city areas who otherwise would not have the financial resources to attend medical school has been an effective way for Texas to address physician shortages in these areas. It is our intent that these policies combined will encourage and support a larger student body to enter a medical career—this larger student body will also better represent the diverse population that Texas must serve.
But larger numbers do not necessarily translate into better quality, and the quality of health care in the United States no longer competes with the world. The United States leads the world in health care spending per capita but trails far behind in the quality of care provided by our well-funded system. Key to addressing the problem of capacity in Texas (and elsewhere) is adequate funding for our medical schools and our training hospitals. Without adequate funding for these institutions we will not have the capacity to expand or diversify our future medical professionals.
In Texas, one way we have increased capacity is by increasing the number of medical institutions. In June 2007, the governor signed legislation approved by the eightieth Texas legislature to fund the final components necessary for the Texas Tech University Health Sciences Center El Paso School of Medicine to become a fully operational four-year medical school. In regards to our teaching hospitals, we have raised our Medicaid rates, created hospital districts with taxing authority, increased appropriations to our indigent county funds, and dedicated $20 million in unclaimed lottery funds to our institutions that provide services to our indigent population.
However, we know we alone cannot address the shortages in and improve the quality of our health care workforce. This is a shared federal and state responsibility. We must work together to provide a comprehensive plan that provides federal support for state implementations of Medicare-funded residency positions, Indirect Medical Education (IME) payments to teaching hospitals, and matching funds for Medicaid support for Graduate Medical Education (GME). Implementing and, more importantly, sustaining our state solutions are far too difficult when state and federal policies do not align. Americans deserve better.
Leticia Van de Putte, Chair, Veteran Affairs and Military Installations Committee, Texas Senate
Children’s Health and Well-Being
The United States has made measurable progress over the past decade in providing health insurance to children through a combination of private insurance and publicly funded child health insurance, notably, Medicaid and the State Children’s Health Insurance Program (SCHIP).
Both health and economic research demonstrates the efficacy of providing health insurance to all children, and the effects of providing health insurance to children are clearly evident in the daily lives of children and their families. Providing access to health care through health insurance typically improves children’s access to preventive care and earlier identification of health issues that are often more resolvable at lesser human and economic cost when identified early on. By familiarizing people with the health care system as children, they will grow with the “health literacy” needed to stay healthy as adults.
While important national progress in providing health insurance to children has been made, there are gaping holes and remarkable disparities in the variances across states of the percentages of children with health insurance. There are alarming disparities in the access to certain types of health care and preventive health care services, such as dental care and behavioral health care. And, there are glaring differences among states in the levels of state tax effort dedicated to covering children’s health care, which cannot be accounted for by the relative per capita income levels of the states.
The United States is within readily achievable striking distance of covering all children with health insurance, leading to the concomitant access to care that most often results. Reinvigorated federal leadership and authentic partnership with the states are called for to achieve health care coverage and access for all children.
The new administration should, within its first two years, provide federal cost-sharing incentives to states based upon the tax effort of states to insure children’s health. Such enhanced incentives should reflect both the states’ per capita income status and the relative tax effort of states to stimulate coverage. Universal health care coverage should start with children first.
Access must be improved for children living in health care workforce shortage areas. Federal investments in health care workforce training and education for institutions as well as individual students in the health professions and allied adjunctive service fields would target these shortages. Workforce, scope of practice, financing, and weakened public health system capacity should be addressed and made a priority in the new administration.
Public health initiatives targeted at children and their parents need to be considerably strengthened and financed. Public health strategies ought to be the hallmarks of the federal government’s approach to improving and assuring the health of our children. Initiatives promoting prenatal care, healthy diets, oral health, exercise, immunizations, and regular check-ups must be expanded and funded.
Schools can and do play a vital role in the provision and coordination of health care. Federal policies should be better coordinated between federal departments and programs in order to financially support and recognize the efficacy of school-based health initiatives.
Diversity and cultural competencies need to be inculcated into the nation’s children’s health and health promotion initiatives as fundamental core aspects. Health disparities must be targeted and mitigated via population-based strategies.
Coordinated information technology systems should be championed and financially encouraged by federal policy to improve access to and portability of children’s health records.
Through a combination of state laws, regulations, and federal Medicaid waivers, approximately one-half of the states do not require “custody relinquishment” by parents in order for their children to have access to ongoing behavioral health care. In the remaining states, parents without adequate health insurance and/or financial means are faced with the painful decision of relinquishing to the state the custody of their child (hence the term “custody relinquishment”). This is done so that their child can receive needed residential and behavioral health care services under the Medicaid program. National leadership to support these caring parents can be achieved by eliminating this custody relinquishment requirement.
Behavioral health care focused on children and their health status needs to be dramatically improved and better coordinated with public education systems. Again, population-based public health strategies and approaches need to be the framework for our behavioral health care initiatives.
The Reforming States Group (RSG) is engaged in key projects focused on the urgency of addressing the health care of children in the custody of states. Two areas of focus of the RSG are addressing the growing use of atypical antipsychotic medication in children and youth (and identifying the “best practices”) and improving the health outcomes of children in state custody. Oral health care is also of major concern to the RSG. Widespread disparate access to all health care has been made even more urgent by the tragic deaths of children unable to access dental care.
Ultimately, to achieve better health care access and better health status for children, the United States needs to cover parents as an essential, linked strategy for children. If parents have health insurance, they will better utilize the health care systems available to their children.
Kevin Concannon, Director, Iowa Department of Human Services
Health Disparities
“Health disparities” is a broad term generally used to describe inequities or gaps in quality of health and health care across gender, ethnic, racial, and socioeconomic groups. Inequities exist in everything from medical coverage to quality of care, access to prescriptions, and general health literacy.
There is no denying the interconnectedness of socioeconomic status, race, ethnicity, and health care, or the resulting poor health outcomes of minorities in the United States. African Americans, Hispanics/Latinos, American Indians, and Native Hawaiians experience higher rates of infant mortality, cardiovascular disease, diabetes, HIV infection/AIDS, and cancer as well as lower rates of immunizations and cancer screenings. Due to these disparities, the National Partnership for Action to End Health Disparities at the U.S. Department of Health and Human Services warns that minority groups in the United States can face a loss of economic opportunities, a decreased quality of life, and an earlier death. The underlying social and economic causes are complex, but two important factors are lack of access to health care and inappropriate or insufficient care.
Methods for reducing or eliminating health disparities within our health care system should focus on increasing the availability of trained interpreters (and training for staff who will interface with those interpreters); improving the recruitment and retention of minorities within the medical professions; involving family members to increase adherence/compliance with treatment; expanding access to quality health insurance coverage for working minorities (and their families); and ensuring that community-based health care services are both accessible and open in the evening hours. Policymakers must also ultimately address the social and economic factors that influence health inequality.
The U.S. Bureau of Labor Statistics predicts that within the next decade 41.5 percent of
the workforce will be composed of members of racial and ethnic minority groups. This statistic
clearly underscores the fact that health inequities among minorities are also a significant issue for the business community.
These gaps in coverage and quality of care affect all minority groups, but none as dramatically as the Hispanic population. In Texas, as in the rest of the United States, we have a rapidly growing Hispanic population, which, sadly, lags behind other groups in regard to access to health care. Hispanics made up 35.7 percent of the Texas population in 2006, according to the Texas State Data Center at the University of Texas at San Antonio. Because the Hispanic population is positioned to become the majority population in Texas, it is crucial that federal, state, and local policymakers work to address the health inequities facing this group.
A major policy challenge affecting all Texans is lack of health insurance coverage; however, Hispanics continue to remain the largest uninsured group in Texas. According to U.S. Census Bureau statistics, approximately 5.7 million Texans were uninsured in 2006, of whom almost 40 percent were Hispanic, by far the largest group. Further, while almost nine out of ten uninsured Latinos or their dependents are workers, Latinos are far less likely than whites to have job-based coverage, regardless of how much they work or the size or nature of the industry in which they work. The problem, therefore, does not primarily lie with the unemployed, but rather, with Hispanic workers unable to obtain coverage through their employers.
Adding to the shortage of health insurance coverage for Hispanics are the lack of access to coverage through publicly sponsored programs for the working population and the inability to reconcile residency and/or citizenship requirements. The U.S. Census Bureau reported 2.48 million non-citizens in Texas, both legal residents and undocumented, and of those, 1.5 million were uninsured. Nationally, 16 percent of U.S. born Hispanic adults reported not having a usual place of health care, while immigrant Hispanic adults were 31 percent more likely to not have a usual place of health care. Most undocumented immigrants, who nationally make up about 26 percent of all foreign-born, are not eligible to receive publicly sponsored coverage, and most legal immigrants must reside for five years before they are eligible to enroll in any government insurance programs. Consequently, a large part of the Hispanic population, both nationally and in Texas, fails to receive health coverage through the workplace or the public sector. Unfortunately, Texas has not been bold in seeking any solutions to our high uninsured rate. Therefore, local communities have been shouldering the cost of uncompensated care in crisis situations.
For those Hispanics fortunate enough to receive health care and coverage, there remains yet another inequity. The quality of health care that Hispanics receive is often lower than that of their white counterparts due to language and cultural barriers. If a health care provider does not speak Spanish fluently, patients are not able to fully understand the diagnoses and treatment instructions given to them. This is a problem not only for the patients and their families but also for the entire health profession team. Physicians know language barriers impede their ability to deliver quality health care, which in turn increases workplace stress. Communication is key between patients and health care professionals for positive outcomes. This “communication gap” between Hispanic patients and their providers only contributes to the inequities the population faces.
Regarding the health disparities facing the Hispanic population resulting from language and cultural differences, lawmakers should consider language concordance initiatives whenever possible, as language concordance has been found to improve communication between Hispanics and their health care providers. Lawmakers should also consider higher-education incentives that target and encourage Hispanic, Spanish-speaking students who plan on practicing health care in areas with high Hispanic populations. Equally important for policymakers to consider is facilitating Spanish language courses and other cultural educational interventions for health care providers. Simple solutions, such as informing physicians of the use of interpreters and the inclusion of family members in medical discussions, have been shown to help clinicians develop Hispanic-specific cultural competency skills.
In sum, addressing health disparities remains a challenge, but lawmakers have a responsibility
to their constituencies to ensure that health care is administered in as fair a manner as possible.
Isn’t it time that discrimination in our health care system be as intolerable as it is in workplace and education settings?
Leticia Van de Putte, Chair, Veteran Affairs and Military Installations Committee, Texas Senate, and Scott Nishimoto, Vice-Chair, Health Committee, Hawaii House of Representatives
Medical Liability Reform
The political history of the medical malpractice issue is one of cyclical bouts of tribal political warfare between doctors and lawyers. The Federal Reserve unwittingly causes the cycles when it raises or lowers interest rates. Because of the long time between when malpractice premiums are paid and the payouts occur, investment earnings from the premiums and reserves are particularly important for medical malpractice insurance. The investments involved are mostly fixed principal, interest earning investments. When interest rates are rising, rising investment earnings keep malpractice premiums stable. When interest rates fall, declining investment earnings cause premiums to rise. This is against a background of rising payments for claims. The costs are, if nothing else, increased by medical inflation raising the cost of the health care needed to correct negligent medical injury.
The medical profession’s standard remedy for malpractice problems is a package of tort reforms based on the California MICRA reforms. MICRA, the 1975 Medical Injury Compensation Reform Act, caps damages and attorneys’ fees. I can’t count the number of times a doctor has told me that “the proven prescription for malpractice is caps.”
If the malpractice problem is narrowly defined as rising insurance premiums, caps do help. They reduce insurance company payouts, which in turn reduces the need for higher premiums. When doctors are using the legal climate to help decide where to locate, having caps makes physician recruitment easier. However, if a broader definition of the malpractice problem is used, caps are an ineffective remedy.
Doctors will recite chapter and verse on the unnecessary tests and procedures they have to do to protect themselves against liability risks. Caps do little to remove the need for this protection—with caps doctors still can and do get sued; the insurance company payout is just not as large.
Of course, someone makes money from doing and interpreting unnecessary tests and procedures. This revenue motivation and the protection from liability are overlapping incentives that together push health care providers to do more than is needed. My thesis is that fixing both of these problems is essential to bringing costs under control—fixing one without the other will have only minor effects.
A side effect of capping awards is that many potential valid malpractice cases are never brought. As noted in a 1991 article by A. Russell Localio and colleagues in the New England Journal of Medicine, a Harvard Medical Practice Study found that less than 2 percent of the cases of medical error resulted in a malpractice complaint being brought. There are numerous reasons for this, but attorneys have said that a case has to have $250,000 in potential damages before they will take it.
Caps also do not correct for improper conclusions to cases. As reported in a 1996 article by Troyen A. Brennan and colleagues in the New England Journal of Medicine, Harvard researchers followed up on fifty-one malpractice claims. They found that in 40 percent of the cases where there was a payout to the plaintiff, there was no malpractice. These cases all ended in settlements, rather than jury verdicts. It was cheaper and safer for the insurance company and doctor to settle rather than fight an unjustified claim. In another third of cases, plaintiffs received nothing despite medical errors having occurred. A further problem is that the justice system is slow. The Harvard study found 10 percent of cases still unresolved eleven years after the event.
The current malpractice system is also very inefficient. Precise data are not available due to the secrecy surrounding the division of the proceeds between the plaintiffs, their attorneys, and court and legal costs (including expert witness fees and expenses), but I have seen estimates of the system taking between 60 percent and 75 percent of all malpractice spending with the injured parties getting between 25 percent and 40 percent.
The current malpractice system is also ineffective as a quality control mechanism. This is not surprising given that the malpractice system never sees the vast majority of the errors, has (what I understand to be) an error rate that is between 40 and 50 percent, and is too slow to provide timely feedback. The threat of malpractice litigation is actually an obstacle to reducing errors because it prevents participants in health care from being open about the errors that do occur. Openness is the first step in identifying the problems so the systems can be redesigned to fix them.
If caps and other MICRA reforms are ineffective, what then is the solution to the malpractice crisis? A family of reforms has been proposed, variously called administrative compensation systems or health courts. The details vary, but the central themes are as follow:
A pure form of this family of reforms has not been tried in the United States. The Wyoming Healthcare Commission found that the Scandinavian countries and New Zealand are using versions of this system successfully.
An example of an administrative compensation system is the Workers’ Compensation system that all fifty states have some version of. In Wyoming, Workers’ Compensation is unpopular with the trial attorneys (it uses their services only on a limited basis with no contingency fees and the state paying the workers’ attorneys on a fixed hourly schedule). It is, however, quite efficient. Wyoming Workers’ Compensation expenses from 1993 through 2007 had administrative and system operating expenses (including legal expenses) of 13.2 percent of the total cost.
Because these proposals use a broader standard of error for compensation and will compensate errors where the damages are too small for the malpractice system, it is not clear whether the direct cost of an administrative compensation system is less or more than the traditional malpractice system. However, it should eliminate the defensive medicine need for unnecessary care. It should also help find and fix the causes of medical error.
Another reform idea, enterprise liability, is a less sweeping reform that may in part meet the needs of the health care systems reformer seeking to control costs. The idea is that a large enterprise takes legal responsibility and the individual medical practitioner is divorced from the expense and fault-finding aspects of malpractice, which should reduce the need for defensive medicine. However, local standards of care and the enterprise itself are likely to mandate some unnecessary practices. Examples of enterprise liability systems include the Federally Qualified Health Centers and the Veterans Health Administration where the federal tort claims system takes responsibility and the individual practitioner is insulated from malpractice costs.
As health care reform advances nationally, states need to take the lead in reforming their malpractice systems. Coverage expansions will focus attention on this issue, and the federal government should take steps to facilitate state action.
Charles Scott, Chair, Labor, Health and Social Services Committee, Wyoming Senate
Medical Liability Reform
During the 2006 session of the Kentucky General Assembly, the House Health and Welfare committee members sat with rapt attention listening to a true horror story being described by a quiet-spoken man who recounted to us his experience with medical error. His testimony was very moving and helped to dampen the mania surrounding tort reform during that session.
Kentucky resident Bill Rogers recounted to us that in 1997, when he was fifty-two years old, he and his wife Lela went to the hospital for a treatable infection on his thigh. Doctors began to treat him with a course of antibiotics. Unfortunately, they were the wrong antibiotics. The infection got worse and spread.
Within a month doctors had to amputate Bill’s penis.
For the past decade, the Commonwealth of Kentucky, just like the rest of the nation, has wrestled with how to make sure individuals who are harmed by medical error are treated in a just and equitable manner. Sadly, the issue has become little more than a political football.
The medical associations and hospitals have lined up with the legislators who demand “tort reform,” while the trial lawyers have lined up with the legislators who believe that the judicial system is not overloaded with frivolous cases and that citizens are entitled to have claims of harmful medical negligence heard by the courts. Each side has accused the other of using this critical issue, deserving of complete apolitical analysis, as a tool to raise funds from the doctors and the lawyers.
Unsurprisingly, we have yet to see an equitable solution to the problem.
The forces who seek to cap damages allege that our state is losing doctors because of the rise in malpractice insurance premiums. Given that Kentucky is already a medically underserved state, it would be madness to drive doctors away.
Kentucky shares a border with Indiana, a state that has imposed limits on damages a person can claim in a lawsuit for medical negligence. Data gathered from the Medical Liability Monitor (October 2006) show that malpractice insurance premiums in Kentucky are rising at below the rate of medical inflation while premiums in Indiana are rising at over double Kentucky’s rate.
As it happens in Kentucky, both the doctors/hospitals and the trial lawyers have been drawn into a controversy without the presence of that crucial third leg of the stool—the medical malpractice insurance industry. So far that industry has eluded examination in the Kentucky debate.
As the debate has evolved, it has become apparent to both the doctors/hospitals and the lawyers that they are mere pawns, which conservatives and liberals bat about like the birdie in an Olympic badminton game.
It is clear that the insurance industry has done a beautiful job of distracting policymakers in Kentucky from focusing on what might be the real reason for increases in medical malpractice premiums.
Kentucky medical malpractice insurance carriers’ annual statements filed each year show that these carriers have paid out significantly less in claims than they estimated they would have to pay.
Our insurance commissioner has no authority to order refunds to doctors who have paid excessive premiums over the years.
Strengthening our oversight regulatory laws on medical malpractice insurance companies in Kentucky needs to be this state’s next investigation.
Whether at the state or federal level, efforts to reform medical liability must educate policymakers about the integral role of the medical malpractice insurance industry, and those efforts must also give state insurance commissioners the necessary tools to fully monitor the malpractice insurance industry and to fix shortcomings in remedies.
Kathy Stein, Chair, Judiciary Committee, Kentucky House of Representatives
About the Authors
John Colmers is secretary of the Maryland Department of Health and Mental Hygiene, an appointee of Democratic Governor Martin O’Malley. Earlier in his career, Colmers spent nineteen years in Maryland state government, where he held various positions, including executive director of the Maryland Health Care Commission and the Health Services Cost Review Commission, the agency overseeing Maryland’s all-payer hospital rate setting system. Colmers is a member of the board of AcademyHealth; he was formerly chairman of CareFirst of Maryland, Inc., an affiliate of CareFirst BlueCross BlueShield. He has a BA from Johns Hopkins University and an MPH from the University of North Carolina at Chapel Hill.
Kevin Concannon is the former director of the Iowa Department of Human Services, an appointee of Democratic Governor Tom Vilsack. He has forty-two years of experience in human services, including heading Maine’s Department of Human Services and Department of Mental Health and Mental Retardation and Oregon’s Department of Human Services. Concannon has also had several national leadership roles, including serving as president of the American Public Welfare Association and the National Association of State Mental Health Program Directors. Concannon holds a BA from St. Francis Xavier University and an MSW degree from St. Francis Xavier University and the Maritime School of Social Work, Dalhousie University.
Gene Davis is a Democratic member of the Utah State Senate where he served as the minority whip and assistant minority whip. He was first elected to the Utah legislature in 1986 and served the first twelve years in the House of Representatives. Davis has been a member of the State Senate since 1998. He is a native of Salt Lake City and has an LLB from LaSalle Extension University.
Bruce Goldberg is director of the Oregon Department of Human Services, an appointee of Democratic Governor Ted Kulongoski. Goldberg’s experience also includes serving as head of the Office for Oregon Health Policy and Research, medical director for CareOregon, health officer for Columbia County in Oregon, and director of community health services in Zuni, New Mexico. He also was a faculty member at Oregon Health and Science University for more than fifteen years. He has published widely and has served on numerous regional and national advisory boards and committees. He is currently chairman of the American Public Human Services Association’s National Policy Council. Goldberg is a graduate of the Mount Sinai School of Medicine and completed his family medicine training at Duke University.
Richard N. Gottfried is a Democratic member of the New York State Assembly where he serves as chair of the Health Committee. First elected to the Assembly in 1970 at the age of twenty-three, he previously served as deputy majority leader; assistant majority leader; chair of the Assembly Codes Committee and the Children and Families Committee; and chair of the Assembly Task Forces on the Homeless, Campaign Finance Reform, and Crime Victims. He is a fellow of the New York Academy of Medicine and a member of the American Public Health Association, the New York Civil Liberties Union, the Association of the Bar of the City of New York, the Art Students League of New York, and the China Institute. Gottfried has a BA from Cornell University and a JD from Columbia Law School.
Jane Kitchel is a Democratic member of the Vermont State Senate where she serves as vice-chair of the Appropriations Committee and co-chair of the Commission on Health Care Reform, which is charged with studying and making recommendations to the legislature on health care reform policy. Kitchel spent thirty-five years in Vermont state government, retiring in 2002 as secretary of the Agency of Human Services. During her tenure working for several governors, she had administrative responsibility for the design and implementation of Vermont’s health care reform initiatives. Currently, she serves on the Vermont Justice for Children Task Force, the Vermont Hunger Task Force, the Vermont Child Poverty Council, and several boards of nonprofit agencies.
Pam Maier is a former Republican member of the Delaware House of Representatives where she chaired the Health and Human Development Committee. She has a BA and a master’s degree in education administration from Oklahoma State University.
S. Peter Mills is a Republican member of the Maine State Senate where he is a member of the Health and Human Services Committee and has also served as a Republican lead on Tax, Labor, Judiciary, and Appropriations Committees for twelve years. He has been practicing law for thirty-two years and is owner of the law firm Wright and Mills in Skowhegan, Maine. Mills is a founding member of the Somerset Economic Development Corporation and a founding member of FirstPark, a successful business park that is bringing over seven hundred jobs to central Maine. He also currently serves on the boards of the Maine Coalition for Excellence in Education and the Maine Children’s Growth Council. Mills received a BA from Harvard College and a JD from the University of Maine School of Law.
Scott Nishimoto is a Democratic member of the Hawaii House of Representatives, where he serves as vice-chair of the Health Committee. His professional experience includes serving as a staff member in the Washington, D.C., office of Senator Daniel K. Inouye and working as a law clerk at Cronin, Fried, Sekiya, Kekina and Fairbanks. He is currently on the board of directors for the Hawaii Children’s Cancer Foundation and is a member of the Hawaii Workforce Development Council. Nishimoto received his BA in sociology from the University of Hawaii and his JD from the University of Hawaii William S. Richardson School of Law. He has been a member of the Hawaii State Bar Association since 2003.
Sandy Praeger is the commissioner of insurance for the State of Kansas. Praeger was formerly president of the National Association of Insurance Commissioners (NAIC). She serves as chair of
the Health Insurance and Managed Care Committee, vice-chair of the International Insurance Relations Committee, member of the Executive Committee for International Association of Insurance Supervisors (IAIS), and a member of other NAIC committees. She was previously elected to the Kansas State Senate in 1992, 1996, and 2000, and before that served one term in the Kansas House of Representatives. Praeger is a graduate of the University of Kansas.
Sybil Richard is deputy secretary of the Louisiana Department of Health and Hospitals, an appointee of Republican Governor Bobby Jindal. Previously, Richard held various positions at the Florida Agency for Health Care Administration, including assistant deputy secretary for Medicaid operations, director of planning and development, and chief of the Bureau of Medicaid Pharmacy Services. From 2001 to 2004, Richard served as the National Association of Chain Drug Stores’ director of federal health programs in Alexandria, Virginia. She also previously served as health policy fellow at the Centers for Medicare and Medicaid Services. Richard has a BS in pharmacy from Xavier University of Louisiana, a master’s degree in health administration, and a law degree from Indiana University.
Elizabeth Roberts is the Democratic lieutenant governor of Rhode Island. She currently serves as chair of the Long Term Care Coordinating Council, the Small Business Advocacy Council, and the Emergency Management Advisory Council. Roberts served in the Rhode Island State Senate from 1997 to 2007 where she was chair of the Senate Health and Human Services Committee and co-chair of the Permanent Joint Committee on Healthcare Oversight. Before serving in the Senate, Roberts worked as a business strategy consultant, policy analyst, and health care manager. Roberts has a BA from Brown University and an MBA in health care management from Boston University.
Charles Scott is a Republican member of the Wyoming State Senate where he was first elected in 1982 and has been chairman of the Committee on Labor, Health and Social Services since 1993. From 2001 to 2004, Scott served as chair or vice-chair of the Health Committee of the National Conference of State Legislatures. Currently, he is a board member of the American Legacy Foundation. He received a BA from Harvard College and an MBA from Harvard Business School.
John Selig is director of the Arkansas Department of Human Services, an appointee of Democratic Governor Mike Beebe. Previously, Selig spent six years as department deputy director and, before that, three years as director of the Division of Mental Health Services. He has served on numerous boards, including the Arkansas Minority Health Commission and the Arkansas Health Services Permit Agency. Selig is a graduate of Stanford University and received a master’s degree in public administration from Princeton University.
Kathy Stein is a Democratic member of the Kentucky State Senate, where she is a member of the Veterans, Military Affairs, and Public Protection Committee. Previously, she served eleven years as a member of the Kentucky House of Representatives. While in the House, she was the chair of the Judiciary Committee—the first woman in Kentucky to ever hold that position. Stein received her law degree from the University of Kentucky College of Law and is an attorney in private practice.
Leticia Van de Putte is a Democratic member of the Texas State Senate where she serves as chair of the Veteran Affairs and Military Installations Committee. A pharmacist for more than twenty-nine years, Van de Putte is also a former five-term state representative. In 2003, she became chair of the Texas Senate Democratic Caucus and was nominated as co-chair of the 2008 Democratic National Convention. She has been actively involved in the National Conference of State Legislatures, serving as president from 2006 to 2007, and she is now serving on the American Legacy Foundation board. Van de Putte was a Kellogg Fellow at Harvard University’s John F. Kennedy School of Government in 1993, and she received her BS from the University of Texas at Austin, College of Pharmacy.
Reforming States Group (RSG) Steering Committee
Thomas C. Alexander
Holly Benson
Linda Berglin
Ned Calonge
Harriette L. Chandler
Eileen L. Cody
John Colmers
Gene Davis
Richard N. Gottfried
Toni Nathaniel Harp
John A. Heaton
Nettie Hoge
Jane Kitchel
Robyn Kruk
S. Peter Mills
Bob Nakagawa
John T. Nilson
Scott Nishimoto
Alan Nunnelee
John M. O’Bannon
Gerry A. Oligmueller*
Janet Olszewski
Sheila Peterson
Sandy Praeger
Sybil Richard
Elizabeth Roberts
Charles Scott
John Selig
Joe Stegner
Kathy Stein
Leticia Van de Putte
Kevin Woods
*ex-officio member
Selected Publications of the Reforming States Group
FEDERALISM IN HEALTH REFORM
1993. The States That Could Not Wait: Lessons for Health Reform from Florida, Hawaii, Minnesota, Oregon, and Vermont. Milbank Memorial Fund.
1994. An Agenda for Federalism from State Leaders, by C. Rydell for the Reforming States Group. Health Affairs 13(5):252–55. Available at http://content.healthaffairs.org/cgi/reprint/13/5/252 (accessed March 16, 2009).
1994. Federalism in Health Reform: Views from the States That Could Not Wait, by H. Nelson. Milbank Memorial Fund.
1994. Five States That Could Not Wait: Lessons for Health Reform from Florida, Hawaii, Minnesota, Oregon, and Vermont, edited by D.M. Fox and J.K. Iglehart. Health Affairs and Milbank Memorial Fund.
1998. Balanced Federalism and Health System Reform, by the Reforming States Group. Health Affairs 17(3):181–91. Available at http://content.healthaffairs.org/cgi/reprint/17/3/181 (accessed March 16, 2009).
1998. The Reforming States Group and the Promotion of Federalism, by K.S. Andersen. The Milbank Quarterly 76(1):103–20. Available at http://www.milbank.org/760104.html (accessed March 16, 2009).
EVIDENCE-BASED HEALTH POLICY
2005. Evidence of Evidence-Based Health Policy: The Politics of Systematic Reviews in Coverage Decisions, by D.M. Fox. Health Affairs 24(1):114–22. Available at http://content.healthaffairs.org/cgi/reprint/24/1/114 (accessed March 16, 2009).
2006. Helping Public Officials Use Research Evaluating Healthcare, by D.M. Fox and L. Greenfield. Journal of Law and Policy 14(2)531–50. Available at http://www.brooklaw.edu/students/journals/bjlp/jlp14ii_fox_greenfield.pdf (accessed March 16, 2009).
2008. Evidence-Based Maternity Care: What It Is and What It Can Achieve, by C. Sakala and M.P. Corry. Childbirth Connection, the Reforming States Group, and the Milbank Memorial Fund. Available at http://www.milbank.org/reports/0809MaternityCare/0809MaternityCare.html (accessed March 16, 2009).
EXPANDING COVERAGE FOR CHILDREN
1998. Expanding Health Coverage for Children: Matching Federal Policies and State Strategies, by K.A. Johnson and J.E. McDonough. Milbank Memorial Fund and the Reforming States Group. Available in print by request. Order online at http://www.milbank.org/order_form.html.
1999. Pediatric Dental Care in CHIP and Medicaid: Paying for What Kids Need, Getting Value for State Payments. Milbank Memorial Fund and the Reforming States Group. Available at http://www.milbank.org/reports/990716mrpd.html (accessed March 16, 2009).
2000. How Federal and State Policy Can Alleviate Children’s Oral Pain, by R. Rawson and D.M. Fox. Journal of the American College of Dentists 67:22–24.
HEALTH INFORMATION POLICY
1999. Public-Private Collaboration in Health Information Policy. Milbank Memorial Fund and the Reforming States Group. Available at http://www.milbank.org/reports/mrinfopolicy.html (accessed March 16, 2009).
PRESCRIPTION DRUG POLICY
2003. State Initiatives on Prescription Drugs: Creating a More Functional Market, by the Reforming States Group. Health Affairs 22(4):128–36. Available at http://content.healthaffairs.org/cgi/reprint/22/4/128 (accessed March 16, 2009).
STATE HEALTH REFORM
2008. A Progress Report on State Health Access Reform, by J.E. McDonough, M. Miller, and C. Barber. Health Affairs—Web Exclusive 29 January w105–w115. Available at http://content.healthaffairs.org/cgi/content/abstract/27/2/w105 (accessed March 16, 2009).
STATE HEALTH EXPENDITURES
1999. 1997 State Health Care Expenditure Report. Milbank Memorial Fund, National Association of State Budget Officers, and the Reforming States Group. Available at http://www.milbank.org/reports/1997shcer/index.html (accessed March 16, 2009).
2001. 1998–1999 State Health Care Expenditure Report. Milbank Memorial Fund, National Association of State Budget Officers, and the Reforming States Group. Available at http://www.milbank.org/reports/1998shcer/index.html (accessed March 16, 2009).
2003. 2000–2001 State Health Care Expenditure Report. Milbank Memorial Fund, National Association of State Budget Officers, and the Reforming States Group. Available online at http://www.milbank.org/reports/2000shcer/index.html (accessed March 16, 2009).
2005. 2002–2003 State Health Expenditure Report. Milbank Memorial Fund, National Association of State Budget Officers, and the Reforming States Group. Available at http://www.milbank.org/reports/05NASBO/index.html (accessed March 16, 2009).
STATE OVERSIGHT OF INTEGRATED HEALTH SYSTEMS
1997. State Oversight of Integrated Health Systems. Milbank Memorial Fund and the Reforming States Group. Available in print by request. Order online at http://www.milbank.org/order_form.html.
1999. Tracking State Oversight of Managed Care. Milbank Memorial Fund and the Reforming States Group. Available at http://www.milbank.org/reports/stateoversight/990918soihs.html (accessed March 16, 2009).
WORKFORCE
2003. Making Sense of the System: How States Can Use Health Workforce Policies to Increase Access
and Improve Quality of Care, by E. Salsberg. Milbank Memorial Fund and the Reforming States Group. Available at http://www.milbank.org/reports/2003salsberg/2003salsberg.html (accessed March 16, 2009).
Selected Publications of the Milbank Memorial Fund
A complete list of the Fund’s reports may be viewed online at www.milbank.org. Single or multiple copies of reports that have print editions are available without charge while supplies last. Most reports are also available electronically on the Fund’s website.
Evidence-Based Maternity Care: What It Is and What It Can Achieve
Medical Regulatory Authorities and the Quality of Medical Services in Canada and the United States
Improving Population Health
Regulating Medical Services in China
Public Housing and Supportive Services for the Frail Elderly: A Guide for Housing Authorities and
Their Collaborators
2005 Robert H. Ebert Memorial Lecture—Emerging and Re-emerging Infectious Diseases:
The Perpetual Challenge
The Future of Academic Medicine: Five Scenarios to 2025
Using Health Research in Policy and Practice: Case Studies from Nine Countries
Evidence-Based Mental Health Treatments and Services: Examples to Inform Public Policy
CALIFORNIA/MILBANK BOOKS ON HEALTH AND THE PUBLIC
The following books are co-published with and distributed by the University of California Press.
For information or to order, call 1-800-777-4726 or visit http://www.ucpress.edu.
Public Health Law: Power, Duty, Restraint—Revised and Expanded Second Edition
The Health Care Revolution: From Medical Monopoly to Market Competition
Searching Eyes: Privacy, the State and Disease Surveillance in America
Low Income, Social Growth, and Good Health: A History of Twelve Countries
State of Immunity: The Politics of Vaccination in Twentieth-Century America
Are We Ready? Public Health since 9/11
Medicare Matters: What Geriatric Medicine Can Teach American Health Care
The Fund also publishes The Milbank Quarterly, a multidisciplinary journal of population health and health policy. Information about subscribing to the Quarterly is available by calling toll-free
1-800-835-6770 or by visiting www.milbank.org/quarterly.
Information about other work of the Fund is available from the Fund at
645 Madison Ave., 15th Floor, New York, NY 10022. Telephone: (212) 355-8400. Fax: (212) 355-8599.
Email: mmf@milbank.org. On the Web: www.milbank.org.
Milbank Memorial Fund The Milbank Memorial Fund is an endowed operating foundation that engages in nonpartisan analysis, study, research, and communication on significant issues in health policy. In the Fund's own publications, in reports, films, or books it publishes with other organizations, and in articles it commissions for publication by other organizations, the Fund endeavors to maintain the highest standards for accuracy and fairness. Statements by individual authors, however, do not necessarily reflect opinions or factual determinations of the Fund.
©2009 Milbank Memorial Fund. All rights reserved. This publication may be redistributed electronically, digitally, or in print for noncommercial purposes only as long as it remains wholly intact, including this copyright notice and disclaimer.
Printed in the United States of America.
Online producer: Stephanie Moe-Quiggle
ISBN 978-1-887748-71-1
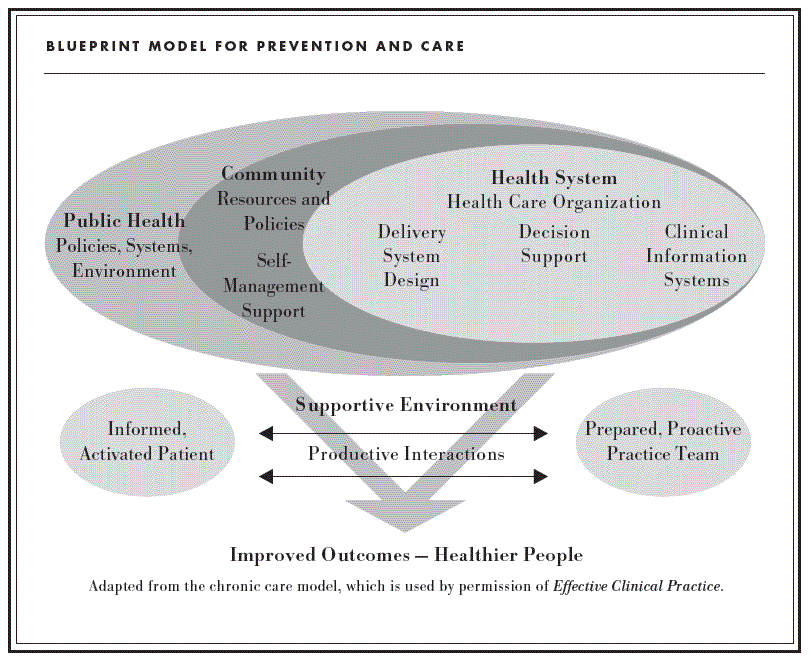
Chair, General Committee
South Carolina Senate
Secretary
Florida Agency for Health Care
Administration
Chair, Health and Human Services
Budget Division
Minnesota Senate
Chief Medical Officer
Colorado Department of Public Health and Environment
Assistant Vice-Chair, Senate Ways and
Means Committee
Massachusetts Senate
Chair, Health Care and Wellness Committee
Washington House of Representatives
Chair Emerita, RSG Steering Committee
Secretary
Maryland Department of Health and
Mental Hygiene
Chair Emeritus, RSG Steering Committee
Minority Whip
Utah Senate
Chair, Health Committee
New York State Assembly
Chair, Committee on Appropriations
Connecticut Senate
Member, Health and Government
Affairs Committee
New Mexico House of Representatives
Policy Director
California Office of the
Lieutenant Governor
Vice-Chair, Appropriations Committee
Vermont Senate
Secretary
Australian Government Department
of the Environment, Water, Heritage and
the Arts
Vice-Chair, RSG Steering Committee
Member, Health and Human
Services Committee
Maine Senate
Co-Chair, RSG Steering Committee
Assistant Deputy Minister,
Pharmaceutical Services
British Columbia Ministry of Health
Member of the Legislative Assembly
Province of Saskatchewan
Chair Emeritus, RSG Steering Committee
Vice-Chair, Health Committee
Hawaii House of Representatives
Chair, Appropriations Committee
Mississippi Senate
Member, Health, Welfare and
Institutions Committee
Virginia General Assembly
Vice-Chair, RSG Steering Committee
State Budget Administrator
Nebraska Department of
Administrative Services
Director
Michigan Department of Community Health
Director, Fiscal Management Division
North Dakota Office of Management
and Budget
Chair Emerita, RSG Steering Committee
Commissioner of Insurance
State of Kansas
Immediate Past President of the National Association of Insurance Commissioners
Chair Emerita, RSG Steering Committee
Deputy Secretary
Louisiana Department of Health and Hospitals
Lieutenant Governor
State of Rhode Island
Co-Chair, RSG Steering Committee
Chair, Labor, Health and Social
Services Committee
Wyoming Senate
Co-Chair, RSG Steering Committee
Director
Arkansas Department of Human Services
Vice-Chair, RSG Steering Committee
Assistant Majority Leader
Idaho Senate
Chair, Judiciary Committee
Kentucky House of Representatives
Chair, Veteran Affairs and Military Installations Committee
Texas Senate
Chair Emerita, RSG Steering Committee
Chief Executive, NHS Scotland
Director-General Health
Scottish Government Health Directorates
by Carol Sakala and Maureen P. Corry
co-published with Childbirth Connection and the Reforming States Group
2008 Available online only
co-published with the Federation of Medical Regulatory Authorities of Canada and the Federation of State Medical Boards
2008 32 pages
by Melissa Sweet and Ray Moynihan
produced in Collaboration with the Centers for Disease Control and Prevention (CDC)
2007 80 pages
by Hong Wang, Yanfeng Ge, and Sen Gong
co-published with the Department of Social Development, Development Research Center (DRC),
the State Council of P.R. China
2007 48 pages
co-published with the Council of Large Public Housing Authorities
2006 Available online only
by Anthony S. Fauci
2006 Available online only
by the International Campaign to Revitalise Academic Medicine
2005 Available online only
by Ray Moynihan
co-published with AcademyHealth
2004 48 pages
by Anthony F. Lehman, Howard H. Goldman, Lisa B. Dixon, and Rachel Churchill
2004 44 pages
by Lawrence O. Gostin
2008 800 pages
$45.00 paper
by Carl F. Ameringer
2008 272 pages
$49.95 cloth
by Amy L. Fairchild, Ronald Bayer, and James Colgrove
2007 368 pages
$50.00 cloth; $19.95 paper; $15.95 Ebook
by James C. Riley
2007 248 pages
$45.00 cloth
by James Colgrove
2006 349 pages
$45.00 cloth
by David Rosner and Gerald Markowitz
2006 210 pages
$18.95 paper
by Christine K. Cassel
2005 269 pages
$35.00 cloth; $16.95 paper; $12.95 Ebook
(To request a bound copy of this report, click here.
Be sure to specify which report you want,
your name, mailing address, and phone number.
To print this report, click here for the pdf version.
To see a complete list of Milbank reports, click here.)
645 Madison Avenue
New York, NY 10022
![]()
![]()
![]()
![]()
![]()
![]()